2022-2023 Impact Report
Our whole system is better because we have designed and adopted a quality system for BC. HQBC is outside the care delivery, it can be objective, it’s not in the day-to-day grind. When we come to this table, we can raise our line of sight. The constitution of the council itself matters, it includes patient, provider, and system leaders to ensure that we have the right voices at the table to do the work.
~ Kathy McNeil, CEO, Island Health


Making the System Safer for Seniors
Jump to Section



Slowing and Stopping Toxic Drug Poisonings
Jump to Section



A Safer System for
Indigenous People
Jump to Section



The Next Generation of Quality Leaders
Jump to Section


Building a Resilient Workforce
Jump to Section
The definition of quality and safety has changed.
Back when they trained us, the determination of quality was how well we thought we did our jobs. We as providers decided if care was appropriate or not.
So the consideration of what matters to patients’ and families, any thoughts around equity, any consideration around indigenous-specific racism, or cultural safety and humility, these things did not exist in our training. The mindset shift has been around patients and families as determiners of their care, and them at the center of deciding what was quality of care or not.
~ Devin Harris, Chair


Making the System Safer for Seniors
123 Quality Improvement Projects enhancing the care of 12,691 seniors attracting 1.4 million in federal investment.
In 2022, the long-term care sector was struggling to recover from the prolonged impacts of the COVID-19 pandemic. There were numerous challenges, including adapting to changing public health guidelines, managing the grief of lost residents, and dealing with recruitment and retention issues among staff.
To help address some of these challenges, a partnership to improve quality in long-term care was established between Health Quality BC (HQBC) and Healthcare Excellence Canada (HEC). This collaboration aimed to expedite the recovery of long-term care homes by providing financial support, coaching, and platforms for knowledge sharing. Last year, the second and third phases of the program supported projects in 123 BC care homes.
The second phase (LTC QI) saw 44 long-term care homes focus on workforce-related issues and the provision of person-centred care. These efforts enhanced the care given to 5,011 seniors. Each participating care home was granted seed funding and access to online educational resources from HEC. Additionally, they received targeted coaching support from HQBC.
For the third phase (Reimagining LTC) a significant priority area was set: each project had to aim to reduce unnecessary prescriptions of antipsychotic medications without a diagnosis. A total of 79 projects were included in this phase, addressing the care of 7,680 seniors. The average target is to reduce unnecessary prescribing by 15%.


Virtual Reality Gives Residents the Chance to Enjoy Life Experiences that Felt Out of Reach
Bringing the outdoors in for assisted living and long-term care residents boosts quality of life and reduces depression.


Dignified Dining for Residents with Swallowing Difficulties
Dan Levitt got the idea to revolutionize food service for seniors while out for dinner with his wife on their anniversary.



Recovering From the Pandemic – Bringing Joy Back to Long-term Care.
In 2022, Accreditation Canada surveyors described Arrowsmith Lodge in Parksville B.C. as “a place where staff want to work, and residents want to live.”
Quality Academy: an Antidote to Health Care Challenges
In 2023, Health Quality BC’s Quality Academy welcomed 39 new graduates to its growing alumni network of 640 dedicated health care professionals across British Columbia. Established a decade ago, the quality improvement learning program transitioned to an online format in 2021, providing asynchronous learning opportunities that were coveted and widely embraced by students amidst the heavy and shifting workloads brought on by the pandemic.
“There is a real tension because when you’re burned out, you can’t just keep going at the same pace and so the instinct can be to just stop. But we can’t stop improvement projects, because I actually think it’s part of the solution. There is evidence that actually giving people things to work on that empower them and motivate them and are aligned with what they value can be energizing. I think quality improvement is the antidote to burnout, not the cause.
Andrew Wray
Quality Academy instructor and
Executive Director at Health Quality BC
Andrew Wray, Quality Academy instructor and Executive Director at Health Quality BC, acknowledged the challenges of exhaustion and burnout among the health care workforce. However, he emphasized the importance of continuing improvement projects as a potential solution to these issues.
This sentiment is echoed by a 2023 Quality Academy graduate who said: “I looked forward to Quality Academy sessions because they were all engaging and applicable to my everyday work, so the time felt worthwhile even though I had other demands. I appreciated having the regular schedule that I could work around, and having dedicated time to reflect, learn and grow weekly in a way that was so relevant to what I do.”
Over six months, students of the Quality Academy Online (QAO) receive 115 hours of lessons and activities, synchronous learning activity forums, project work, coaching and mentoring.
QAO has graduated 95 students since 2021.
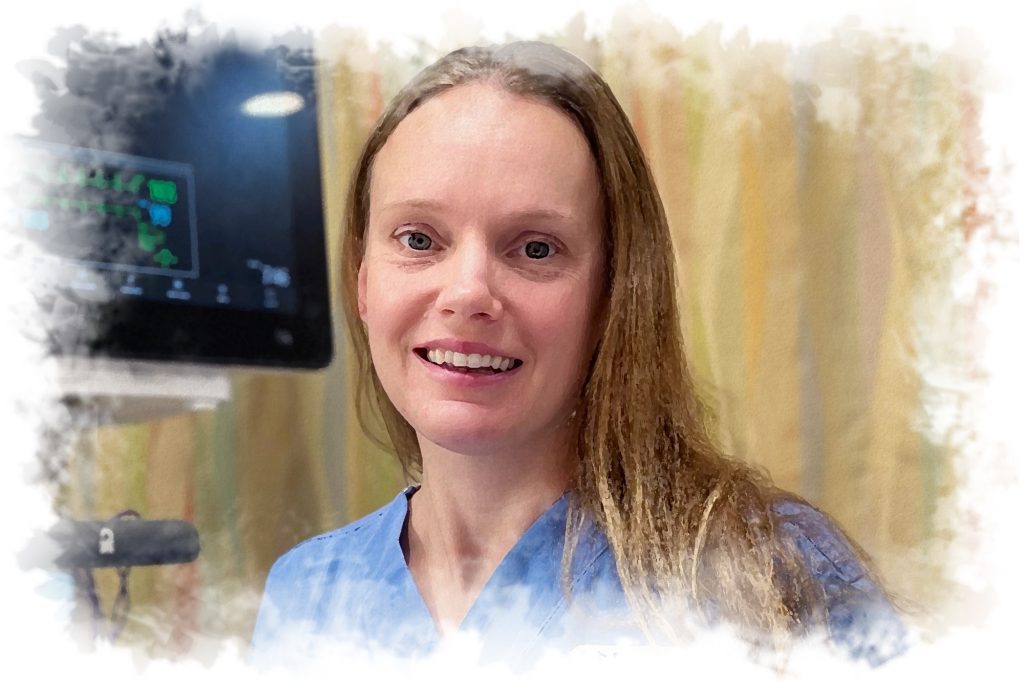

Quality Academy Delirium Project Leads to Better Patient Outcomes



Quality Academy Graduate Brings Cutting-edge Cleaning Procedures to Fraser Health Medical Device Reprocessing
Sharan Kaur signed up for the Quality Academy Online because she saw an opportunity to learn, grow, make meaningful improvements, and inspire her colleagues.


The Gift of Sight Given Sooner
Quality improvement project aims at reducing the time between a donor’s passing and the release of corneal tissue.
Slowing and Stopping Toxic Drug Poisonings
On April 14, 2016, Provincial Health Officer Dr. Perry Kendall declared a Public Health Emergency under the Public Health Act due to the unprecedented rise in deaths due to toxic drug poisonings in British Columbia. While significant improvements in care have been made since this declaration, the number of people dying in BC has continued to rise.
Improving access to appropriate and effective treatments and supports is critical to preventing toxic drug poisonings before they happen. Through Learning about Opioid Use Disorder (LOUD) collaboratives, capability development within Community Action Teams, and substance use journey mapping sessions, we are supporting improvements in care for people who use opioids. Here is some of the work we did this year:
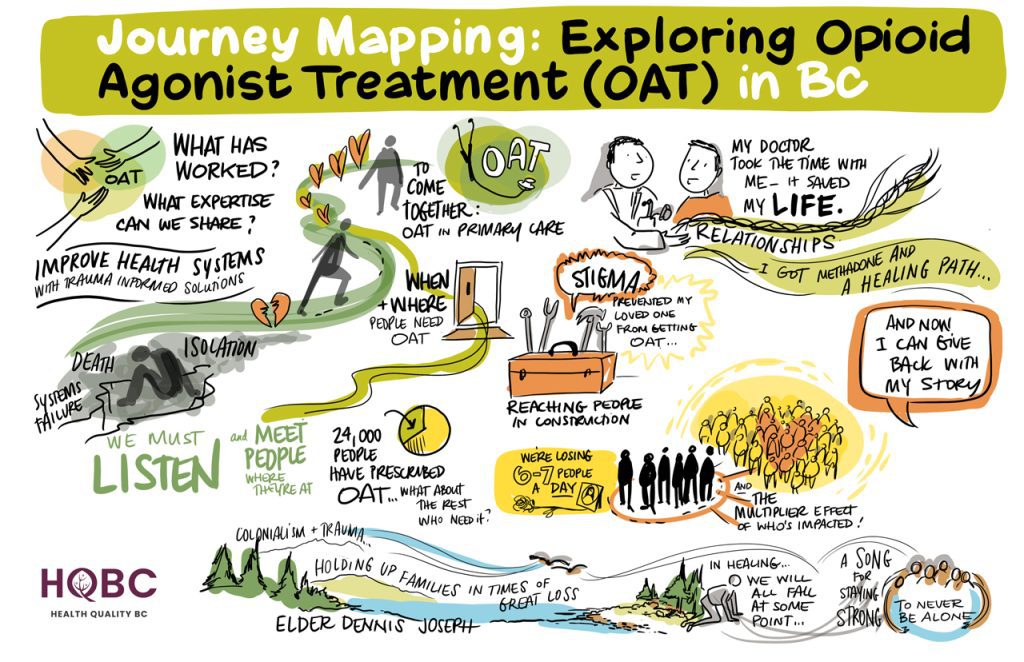

LOUD Collaboratives
Learning about Opioid Use Disorder (LOUD) collaboratives are quality improvement initiatives focused on care for people who use opioids through increasing access to Opioid Agonist Therapy (OAT) in primary care and emergency department settings. This year, we invited health care partners and people with lived experience to participate in a journey mapping session, so we could learn about their experience accessing care, which will better inform work we’ll be leading to provide high-quality primary care for people who use drugs in our communities.


CAT Knowledge Exchange
Community Action Teams (CATs) are an integral part of responding to the toxic drug crisis in BC. The CAT Knowledge Exchange connects all 36 CATs throughout BC to share learning and accelerate local work to address the crisis. Support included capacity building webinars as well as project-focused sessions on anti-stigma, overdose prevention sites and safer supply.



Health Quality BC Partners With Peers and Providers to Spread the Facts on Safer Supply
When Kenn Quayle’s family doctor retired at the height of the COVID-19 pandemic, Quayle was abruptly cut off from his safe supply of prescription opioids.
A Safer System for Indigenous People
At Health Quality BC, and in support of Section 1.1.1 of the BC Cultural Safety and Humility Standard, we are committed to ensuring our organization’s actions are actively in resistance to Indigenous-specific racism.
We actively took steps toward this by establishing an Indigenous Health team in September 2022. This team upholds HQBC’s ongoing commitment to cultural safety and humility by leveraging our unique role within the health care system to advise and support conversations on cultural safety and Indigenous-specific racism work. It also supports HQBC’s leadership and staff by providing an Indigenous perspective within our Strategic Plan, leadership in implementing the Cultural Safety and Humility Standard and recommendations from the In Plain Sight report, consultation on initiatives where Indigenous populations are/will be impacted, and informing the work of cultural safety and anti-racism across the organization.
Towards these, in 2022-23 the Indigenous Health team co-hosted dialogues about cultural safety and humility education and training and became a key support of the work of the Indigenous Board Members Network. It also guided conversations with Indigenous Peoples in the development of the Sharing Concerns Guide, which established principles for an Indigenous Patient Feedback Process, a first of its kind in Canada. The principles support recommendation 5 in the In Plain Sight report, which recognized the need to support a safer way for Indigenous people to share concerns about their health care experiences.
Read on to learn more about the work we did this year to address cultural safety and resist Indigenous-specific racism.


Untangling Colonial Knots: Addressing Anti-Indigenous Racism in Health Care
Sharing Concerns Guide offers a foundation for health partners to receive Indigenous feedback.



HQBC Hosts the Indigenous Board Network
Diane Jules has been involved in health systems transformation for more than 25 years, including seven years as a member of Interior Health’s Board of Directors.
Caring for Workers so They Can Care for Patients
The impacts of the many crises we’ve experienced in recent years are beginning to show – in our families, our schools, and our communities. Few have felt those impacts like BC’s health care workers, who faced the pandemic, wildfires and floods from the front lines.
With support from the Rural Coordination Centre of BC, we talked to health care workers around the province as a way to honour and bear witness to their experiences, and to express our immense appreciation for them.
We unveiled their stories at Quality Forum 2022 in the video Caring Unmasked. It had a far greater impact than we ever imagined it would. It allowed people to feel seen, to reflect on the past few years, and to heal.
Watch Caring Unmasked, and hear from those who lived through our crises and kept us safe. Together we will heal, and we will emerge stronger.
All of us were terrified that we would be the person to bring COVID into the facility.
Sandra Smith
Health Care Aide
Fraser Hope Lodge,
Fraser Health (4:44)
Being in the long-term care facility you don’t know how much longer some of these residents have so it could be the last time they (their family) talk to them and it’s through a window….
Trisha Hart
…In a long-term care facility when they (residents) pass you grieve for them, just like their family does.
Housekeeping
The Summit Long term Care home
Island Health
Having sufficient build-up of just trauma and you’re no longer who you once were. If you don’t take time to remember who that is and replenish it then your just not going to be the provider you set out to be, and you can’t help the sheer number of people you could have if you did take the time to take care of yourself.
Vicky Alfred
Primary Care Paramedic
BC Ambulance Station 248
There’s a component of duty and what we signed up to do as health care professionals, to be there for our patients when they need us no matter what.
David Sweet
Critical Care Physician
Vancouver General Hospital
There were days when we would design something in the morning then it would change at lunchtime and then by evening there was a third message going out…
Allison Muniak
…And looking out this window at 7 o’clock, we were still here at working and seeing the police cars and fire trucks, there must have been 50 of them in a row, and all the people in the community outside, it was amazing to just see the support. It was impactful.
Executive Director Quality and Patient Safety, Infection Prevention and Control and Risk Management
Vancouver Coastal Health
This has been such a sustained period of time so you have to be on, you know you have to keep the pace, you have to stuff your feelings because there is work to do…
Dr. Nel Wieman
…There came a point where I definitely recognized within myself the need to change how I was working. Because we were all working like that and everyone is like ‘Well I’m doing fine, are you doing fine? I’m fine.’ Meanwhile, everyone is saying to each other we can’t sustain this. This pace of work is unsustainable.
Deputy Chief Medical Officer
First Nations Health Authority
I remember talking to one of my colleagues and realizing that I sounded really burned out. That most of what came out of my mouth was negative. Most of what I was thinking was negative and I couldn’t shake it….
Devin Harris
….Thanks to COVID I think what we have really learned about the health care workforce is that we have to take time for ourselves and that we have to recognize that there was a lot of pressure on our nurses and doctors and other staff in filling gaps in health care.
Emergency Room Physician, Kelowna General Hospital. Executive Medical Director Quality & Safety
Interior Health

